COMPREHENSIVE TEXTBOOK OF OBSTETRICS AND GYNECOLOGY (OBG)
नमस्ते साथियों! Bexyhub पर आप सभी का स्वागत है। मेरा नाम दीपक कुमार (Nursing Officer) है। आज के इस आर्टिकल में हम नर्सिंग के एक बहुत ही महत्वपूर्ण टॉपिक के बारे में विस्तार से चर्चा करेंगे। यह नोट्स विशेष रूप से नर्सिंग छात्रों और मेडिकल एग्जाम्स की तैयारी कर रहे साथियों के लिए सरल भाषा में तैयार किए गए हैं। चलिए शुरू करते हैं
Chapter 1: Anatomy and Physiology of Female Reproductive System
The female reproductive system is divided into external and internal organs.
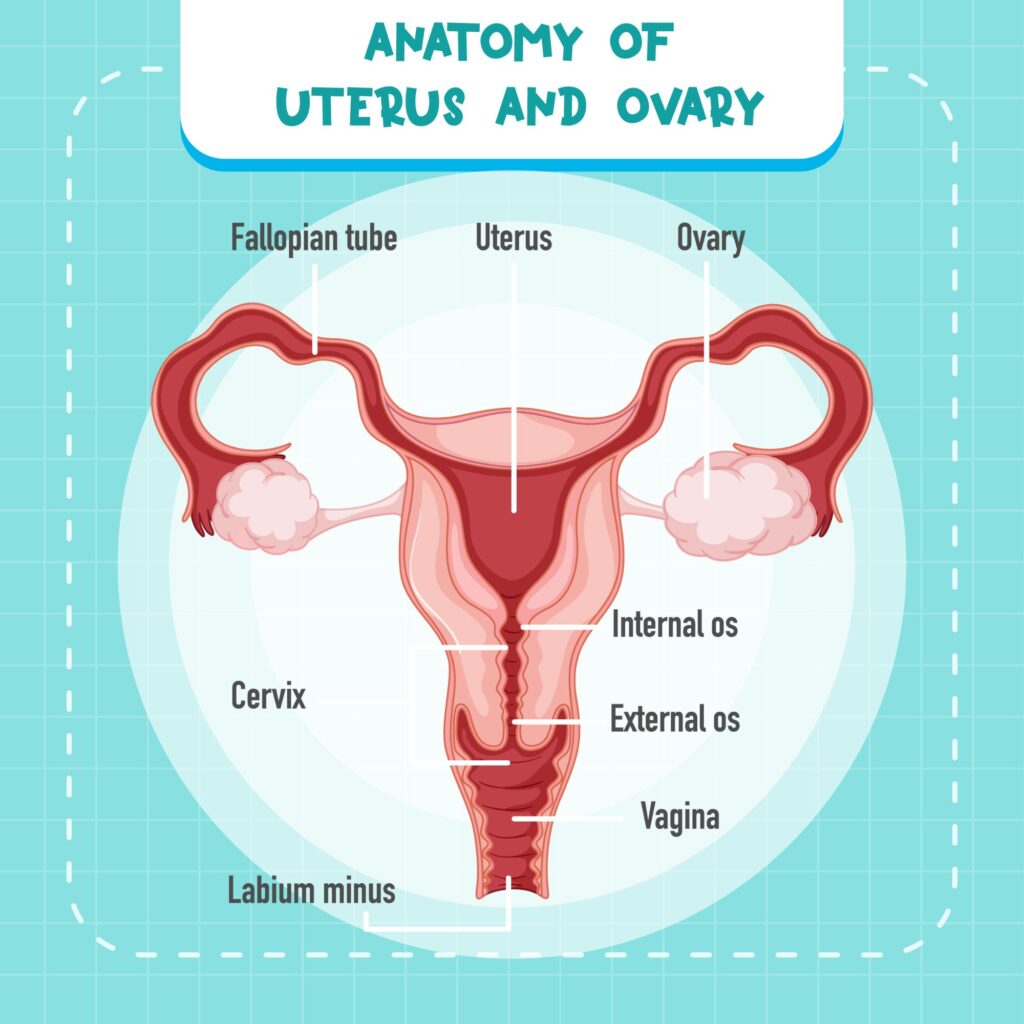
The external organs (Vulva) include the Mons Pubis, Labia Majora, Labia Minora, Clitoris, and Vestibule. The internal organs comprise the Vagina, Uterus, Fallopian Tubes, and Ovaries.
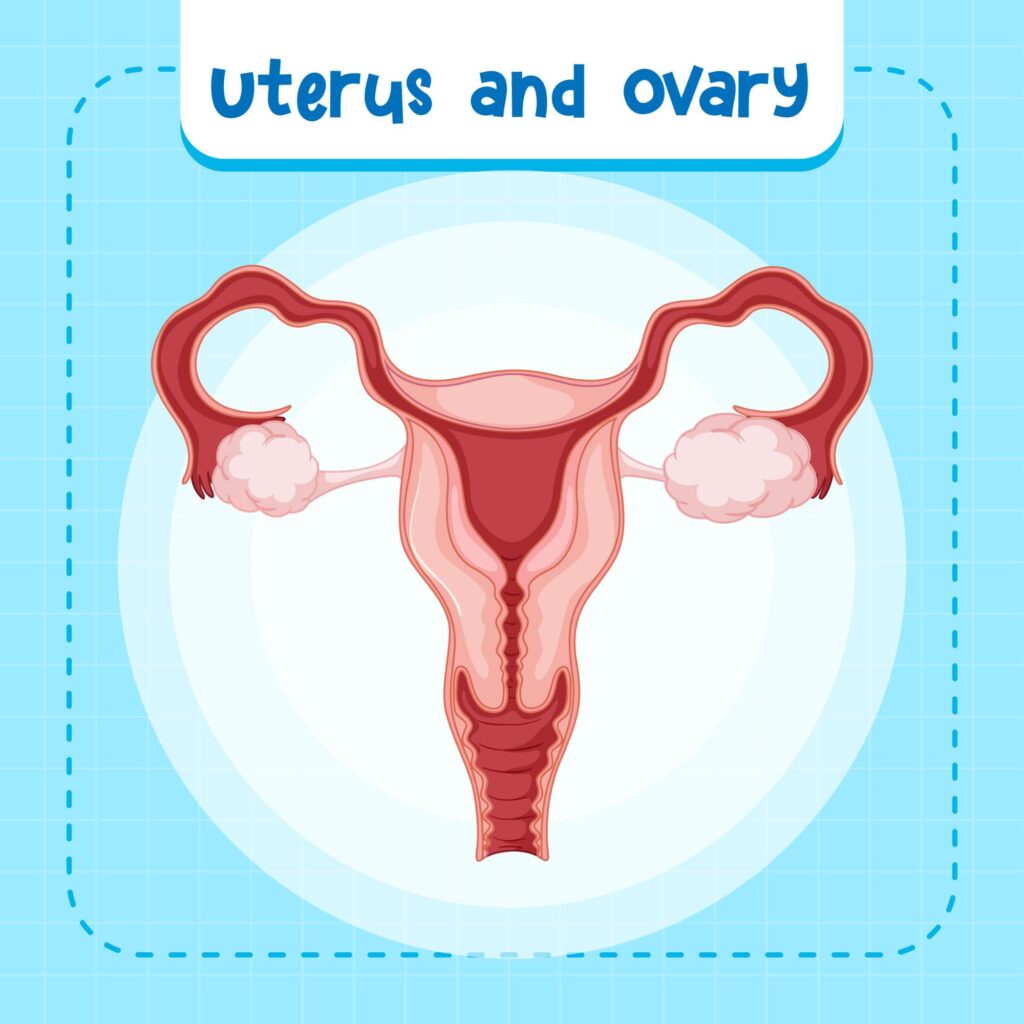
The Uterus is a hollow, pear-shaped muscular organ located in the pelvic cavity between the bladder and the rectum. Its primary function is to nourish the developing fetus.
The Ovaries produce ova and secrete hormones, primarily Estrogen and Progesterone. The Fallopian tubes serve as the pathway for the ovum and the site for fertilization.
Chapter 2: Menstrual Cycle and Gametogenesis
The menstrual cycle is a repetitive monthly cycle that prepares the female body for pregnancy.
It consists of the Ovarian cycle (Follicular, Ovulation, and Luteal phases) and the Uterine cycle (Menstrual, Proliferative, and Secretory phases).
Ovulation occurs around day 14. Gametogenesis involves Oogenesis in females and Spermatogenesis in males.
Fertilization typically occurs in the ampulla of the fallopian tube, leading to the formation of a zygote.
Chapter 3: Fetal Development and Placenta
Following fertilization, the zygote undergoes cleavage and becomes a blastocyst, which implants in the uterine wall. The period of development is divided into the embryonic period (up to 8 weeks) and the fetal period (9 weeks to birth).
The Placenta is a temporary organ that facilitates nutrient exchange, waste removal, and gas exchange between mother and fetus.
It also produces Human Chorionic Gonadotropin (hCG), which maintains the pregnancy in the early stages.
Chapter 4: Physiological Changes During Pregnancy
Pregnancy induces systemic changes in the mother. The blood volume increases by nearly 50%, leading to physiological anemia.
The heart rate and cardiac output increase. Respiratory rate slightly increases as the growing uterus elevates the diaphragm.
Skin changes include Chloasma (the mask of pregnancy) and Linea Nigra. Musculoskeletal changes often result in lordosis (backward leaning) to maintain balance.
Chapter 5: Antenatal Care (ANC)
Antenatal care is the comprehensive medical supervision provided to a pregnant woman. It aims to detect potential complications early.
Key components include regular blood pressure monitoring, weight checks, and abdominal examinations to assess fundal height and fetal heart sounds.
Screening tests for syphilis, HIV, and gestational diabetes are standard. Tetanus Toxoid (TT) immunization is provided to prevent neonatal tetanus.
Chapter 6: Normal Labor and Delivery (Intrapartum Care)
Labor is the process by which the fetus, placenta, and membranes are expelled.
First Stage: Involves cervical effacement and dilation until it reaches 10 cm.
Second Stage: Begins at full dilation and ends with the birth of the baby.
Third Stage: Involves the separation and expulsion of the placenta.
Fourth Stage: A critical observation period of 1 to 2 hours post-delivery to monitor for hemorrhage.
Chapter 7: Complications of Pregnancy (High-Risk Obstetrics)
Common complications include:
Hypertensive Disorders: Preeclampsia (high BP and proteinuria) and Eclampsia (convulsions).
Antepartum Hemorrhage (APH): Bleeding after 28 weeks, caused by Placenta Previa or Abruptio Placentae.
Gestational Diabetes Mellitus (GDM): Carbohydrate intolerance first recognized during pregnancy.
Multiple Pregnancy: Carrying more than one fetus, which increases the risk of preterm labor.
Chapter 8: Postpartum Period (Puerperium)
The Puerperium starts after the delivery of the placenta and lasts for 6 weeks. During this time, the uterus undergoes “involution” to return to its pre-pregnancy size. Vaginal discharge, called Lochia, progresses from Rubra (red) to Serosa (pink) to Alba (white).
Postpartum Hemorrhage (PPH) is a major risk, defined as blood loss exceeding 500 ml in a vaginal delivery.
Chapter 9: Gynecological Disorders
This chapter covers conditions affecting the non-pregnant reproductive system:
Menstrual Disorders: Amenorrhea (absence), Menorrhagia (heavy), and Dysmenorrhea (painful).
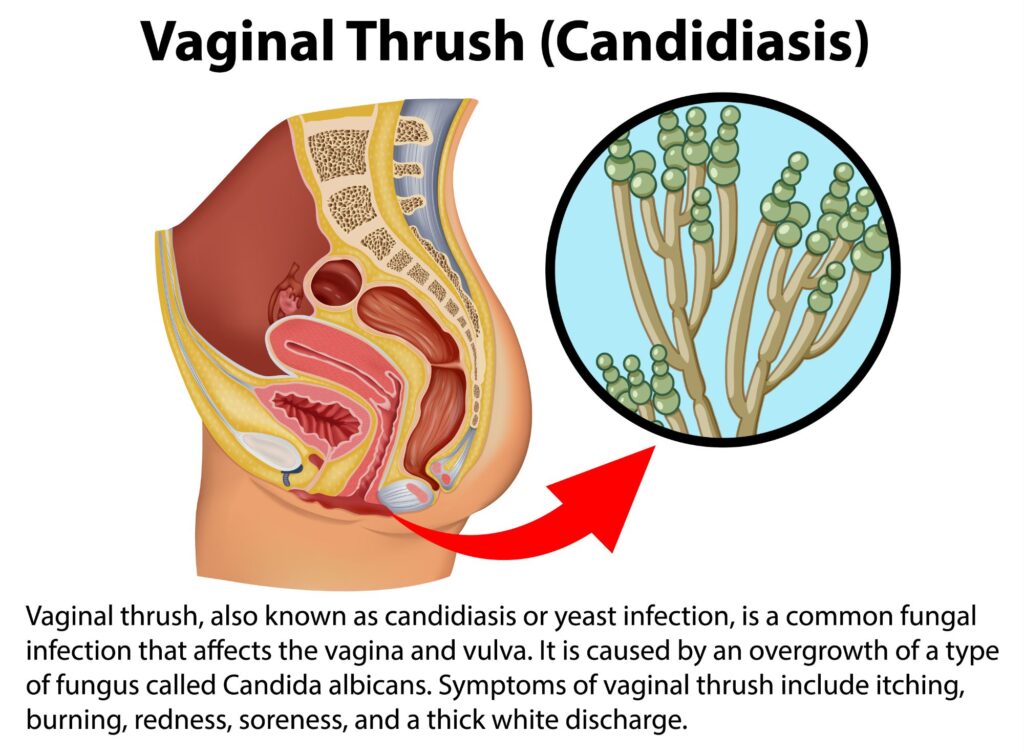
Infections: Pelvic Inflammatory Disease (PID) and various forms of Vaginitis.
Tumors: Uterine fibroids (benign) and various cancers (Cervical, Ovarian, Endometrial).
PCOS: A hormonal disorder causing enlarged ovaries with small cysts.
Chapter 10: Contraception and Infertility
Contraception methods include barrier methods, hormonal pills, Intrauterine Contraceptive Devices (IUCDs) like Copper T, and permanent sterilization (Tubectomy/Vasectomy). Infertility is the inability to conceive after one year of regular unprotected intercourse.
Management includes ovulation induction, intrauterine insemination (IUI), or In-Vitro Fertilization (IVF).
Chapter 11: Fetal Skull and Maternal Pelvis
The study of the fetal skull is vital for understanding the mechanism of labor.
The skull is divided into the vault, face, and base. Important landmarks include the fontanelles (Anterior/Bregma and Posterior/Lambda) and sutures (Sagittal, Coronal, and Frontal).
These allow for “molding”—the overlapping of skull bones to fit through the birth canal.
The maternal pelvis is categorized into four types: Gynecoid (most favorable for delivery), Android (male-like), Anthropoid, and Platypelloid.
The “true pelvis” is the bony canal through which the baby must pass, and its diameters (Inlet, Cavity, and Outlet) determine the success of vaginal delivery.
Chapter 12: Mechanism of Normal Labor (Vertex Presentation)
This is a series of passive movements the fetus undergoes during its passage through the birth canal. It follows a specific sequence:
Engagement: The largest diameter of the fetal head enters the pelvic inlet.
Descent: Continuous movement throughout labor.
Flexion: The chin touches the chest to present the smallest diameter.
Internal Rotation: The head rotates so the occiput is under the symphysis pubis.
Extension: The head is born by extension as it emerges from the vulva.
Restitution & External Rotation: The head aligns with the shoulders.
Expulsion: The rest of the body is delivered.
Chapter 13: Pharmacology in Obstetrics
A Nursing Officer must be expert in “OBG Drugs.”
Oxytocin: Used to induce or augment labor and to prevent/treat Postpartum Hemorrhage (PPH) by stimulating uterine contractions.
Magnesium Sulfate (MgSO_4): The drug of choice for preventing and treating seizures in Eclampsia. Nurses must monitor for toxicity (loss of knee-jerk reflex, respiratory rate below 12).
Misoprostol & Methylergometrine: Used to manage the third stage of labor and control bleeding.
Tocolytics (e.g., Nifedipine): Used to stop premature labor contractions.
Chapter 14: Induction and Augmentation of Labor
Induction is the artificial initiation of labor before it begins spontaneously, whereas augmentation is the stimulation of contractions when spontaneous labor is inadequate.
Common methods include:
Cervical Ripening: Using Prostaglandin gels (PGE2).
Amniotomy (ARM): Artificial Rupture of Membranes using an amnihook.
Oxytocin Infusion: Carefully titrated via an IV pump.
Bishop Score: A pre-procedure assessment to determine if the cervix is “ripe” or ready for induction.
Chapter 15: Operative Obstetrics
When vaginal delivery is not possible or safe, operative methods are used:
Episiotomy: A surgical incision of the perineum to enlarge the vaginal opening during the second stage of labor.
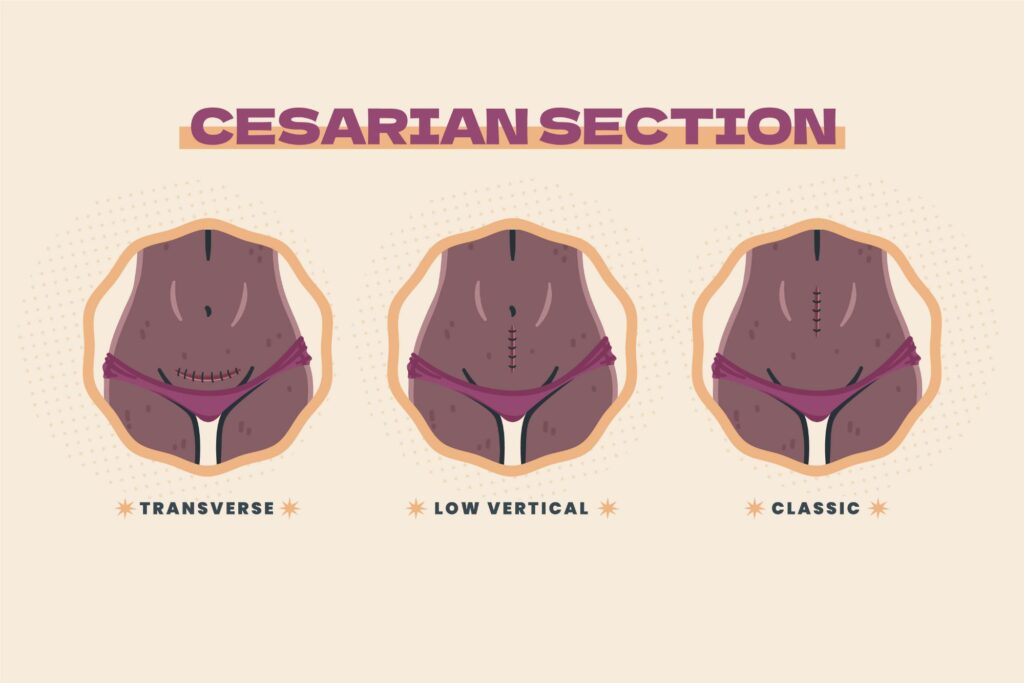
Cesarean Section (LSCS): The delivery of the fetus through an abdominal and uterine incision. Common indications include fetal distress, cephalopelvic disproportion (CPD), or previous C-sections.
Instrumental Delivery: The use of Forceps or a Vacuum Extractor (Ventouse) to assist in the expulsion of the fetal head.
Chapter 16: Neonatal Care and Resuscitation
Immediate care after birth is critical. This includes:
Apgar Score: Taken at 1 and 5 minutes to assess Heart Rate, Respiratory Effort, Muscle Tone, Reflex Irritability, and Color.
Thermoregulation: Keeping the baby warm to prevent cold stress.
Cord Care: Clamping and cutting the umbilical cord.
Resuscitation: If the baby does not breathe immediately, the “ABC” (Airway, Breathing, Circulation) protocol is followed, often involving tactile stimulation, suctioning, or positive pressure ventilation.
Chapter 17: Fetal Wellbeing and Surveillance
Monitoring the health of the fetus during pregnancy and labor is critical to preventing stillbirth and neonatal distress.
Fetal Kick Count: The mother tracks movements; a significant drop (less than 10 kicks in 2 hours) requires medical attention.
Non-Stress Test (NST): A non-invasive test where fetal heart rate (FHR) is monitored in response to fetal movement. A “Reactive” result is a sign of good health.
Biophysical Profile (BPP): Combines NST with ultrasound to check fetal breathing, movement, tone, and amniotic fluid volume.
Cardiotocography (CTG): Continuous monitoring of FHR and uterine contractions during labor. Key patterns include “Accelerations” (good) and “Decelerations” (potential distress).
Chapter 18: Abnormalities of the Placenta and Cord
Disorders of the “support system” can lead to life-threatening emergencies.

Placenta Accreta/Increta/Percreta: Conditions where the placenta attaches too deeply into the uterine wall, leading to severe hemorrhage during delivery.
Vasa Previa: Fetal blood vessels cross the internal os of the cervix, risking rupture during labor.
Cord Prolapse: The umbilical cord slips into the vagina ahead of the baby. This is a surgical emergency because the baby’s head can compress the cord, cutting off oxygen.
True vs. False Knots: True knots in the umbilical cord can cause fetal death if they tighten.
Chapter 19: Obstetric Emergencies and Nursing Management
As a Nursing Officer, you must recognize these “Red Flags” immediately:
Shoulder Dystocia: The head is delivered but the shoulders are stuck. Nurses assist with the McRoberts Maneuver (pulling the mother’s thighs toward her abdomen) and Suprapubic Pressure.
Uterine Inversion: The uterus turns inside out, usually due to improper traction on the umbilical cord.
Amniotic Fluid Embolism: A rare but fatal condition where amniotic fluid enters the mother’s bloodstream, causing sudden respiratory failure and shock.
Shock in Obstetrics: Managing hypovolemic shock (due to bleeding) and septic shock (due to infection).
Chapter 20: Puerperal Sepsis and Postnatal Infections
Infections following childbirth are a major cause of morbidity.
Puerperal Pyrexia: A temperature of 38°C (100.4°F) or higher on any two of the first ten days postpartum (excluding the first 24 hours).
Endometritis: Inflammation of the inner lining of the uterus, characterized by foul-smelling lochia and pelvic pain.
Mastitis: Infection of the breast tissue, often caused by a blocked milk duct. Nurses must encourage continued breastfeeding or pumping to clear the infection.
Deep Vein Thrombosis (DVT): Increased risk of blood clots in the legs after delivery; early ambulation is the best prevention.
Chapter 21: Gynecology – Pelvic Organ Prolapse
Weakness of the pelvic floor muscles causes organs to drop from their normal position.
Cystocele: The bladder bulges into the vagina.
Rectocele: The rectum bulges into the vagina.
Uterine Prolapse: The uterus descends into the vaginal canal.
Management: Use of Pessaries (removable devices) or surgical repair such as Hysterectomy or Pelvic Floor Repair.
Chapter 22: Benign and Malignant Lesions of the Uterus
Uterine Fibroids (Leiomyomas): Benign tumors of the muscle layer. Symptoms include heavy bleeding and pressure.
Cervical Cancer: Highly preventable through HPV vaccination and regular Pap smears.
Endometrial Cancer: Most common in postmenopausal women; the primary symptom is abnormal vaginal bleeding.
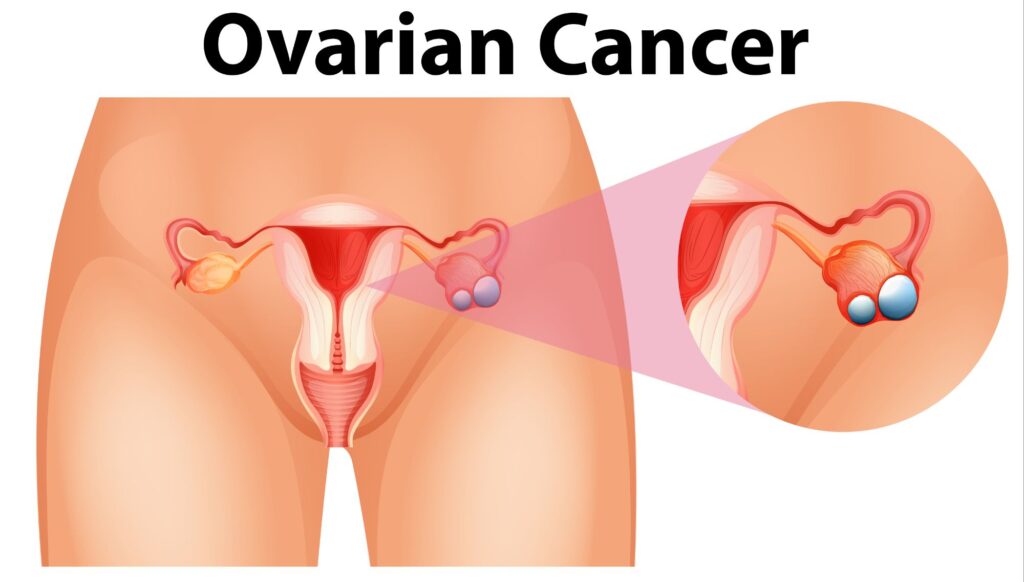
Ovarian Cancer: Often called the “Silent Killer” because symptoms (bloating, pelvic pain) appear only in advanced stages.
Chapter 23: Diagnostic Imaging and Procedures in OBG
Modern obstetrics relies heavily on technology to visualize the health of the mother and fetus.
Ultrasonography (USG): The gold standard. Transvaginal (TVS) is used in early pregnancy, while Transabdominal is used later. It assesses fetal age, placental position, and amniotic fluid index (AFI).
Hysterosalpingography (HSG): An X-ray procedure used primarily in infertility cases to check if the fallopian tubes are open (patent).
Amniocentesis: Withdrawing amniotic fluid (usually around 15–20 weeks) to test for chromosomal abnormalities like Down Syndrome.
Colposcopy: A detailed examination of the cervix using a magnifying instrument, usually performed if a Pap smear shows abnormal cells.
Chapter 24: Social Obstetrics and National Health Programs
As a Nursing Officer in India, understanding government initiatives is essential for public health questions.
Janani Suraksha Yojana (JSY): A safe motherhood intervention to reduce maternal and neonatal mortality by promoting institutional delivery among poor pregnant women.
Janani Shishu Suraksha Karyakram (JSSK): Entitles all pregnant women delivering in public health institutions to absolutely free and no-cost delivery, including C-sections.
Maternal Mortality Rate (MMR): Defined as the number of maternal deaths per 100,000 live births. The leading cause globally is Hemorrhage.
Infant Mortality Rate (IMR): The number of deaths of infants under one year of age per 1,000 live births.
Chapter 25: Legal and Ethical Issues in OBG
Medical-legal knowledge is a frequent topic in nursing officer competitive exams.
MTP Act (Medical Termination of Pregnancy): Legal guidelines for abortion in India. It was amended in 2021 to allow termination up to 24 weeks for specific categories of women (with medical board approval for beyond 24 weeks in cases of fetal anomalies).
PCPNDT Act: The Pre-Conception and Pre-Natal Diagnostic Techniques Act, which strictly prohibits sex determination of the fetus to prevent female feticide.
Informed Consent: The legal requirement for a nurse/doctor to explain the risks and benefits of a procedure (like a C-section or Tubectomy) and obtain a signed agreement from the patient.
Chapter 26: Nursing Management and Documentation
The “Human Version” of nursing care involves more than just medicine; it involves the process of care.
Partograph: A composite graphical record of key data (fetal heart rate, cervical dilation, maternal vitals) during labor. It helps in the early identification of prolonged or obstructed labor.
Nursing Diagnosis in OBG: Examples include “Acute pain related to uterine contractions” or “Risk for deficient fluid volume related to postpartum hemorrhage.”
Documentation: Accurate recording of the time of birth, Apgar scores, and the timing of medication administration (especially Oxytocin and MgSO_4).
Chapter 27: Menopause and Post-Reproductive Health
Menopause: Defined as the permanent cessation of menstruation for 12 consecutive months, usually occurring between ages 45–55.
Symptoms: Hot flashes, night sweats, vaginal dryness, and mood swings due to decreased Estrogen.
Health Risks: Increased risk of Osteoporosis (brittle bones) and Cardiovascular diseases.
Hormone Replacement Therapy (HRT): Medical treatment involving estrogen and progesterone to relieve symptoms, though it carries risks that must be managed.
Chapter 28: Disorders of the Newborn
A Nursing Officer must be able to identify neonatal emergencies immediately following birth.
Neonatal Jaundice: Yellowish discoloration of the skin and eyes due to high bilirubin levels. Physiological jaundice appears after 24 hours, while Pathological jaundice appears within the first 24 hours and is more serious.
Respiratory Distress Syndrome (RDS): Common in preterm babies due to a deficiency of “Surfactant,” which keeps the lung alveoli open.
Birth Injuries: Conditions like Caput Succedaneum (swelling of the scalp that crosses suture lines) and Cephalhematoma (bleeding under the scalp that does not cross suture lines).
Congenital Anomalies: Identifying Neural Tube Defects (like Spina Bifida), Cleft Lip/Palate, and Imperforate Anus during the initial head-to-toe assessment.
Chapter 29: Infertility and Assisted Reproductive Technology (ART)
Infertility affects approximately 10-15% of couples. Nursing management involves emotional support and technical assistance.
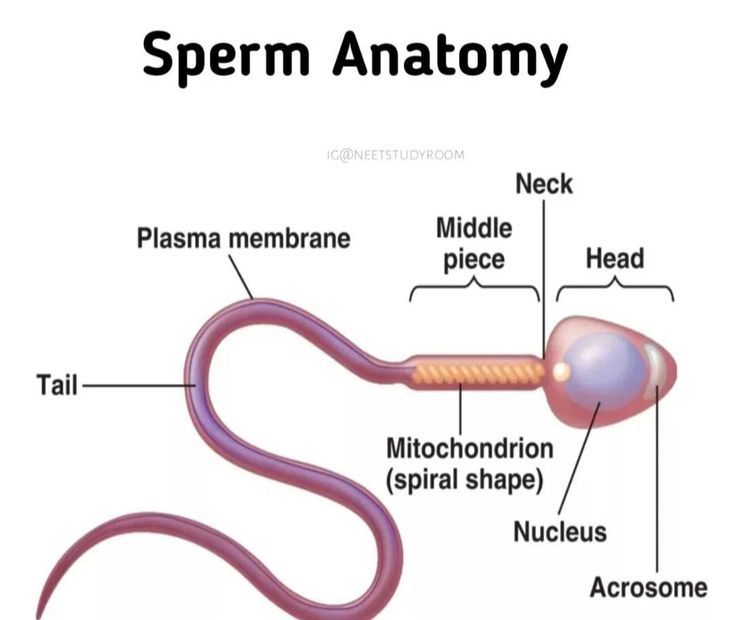
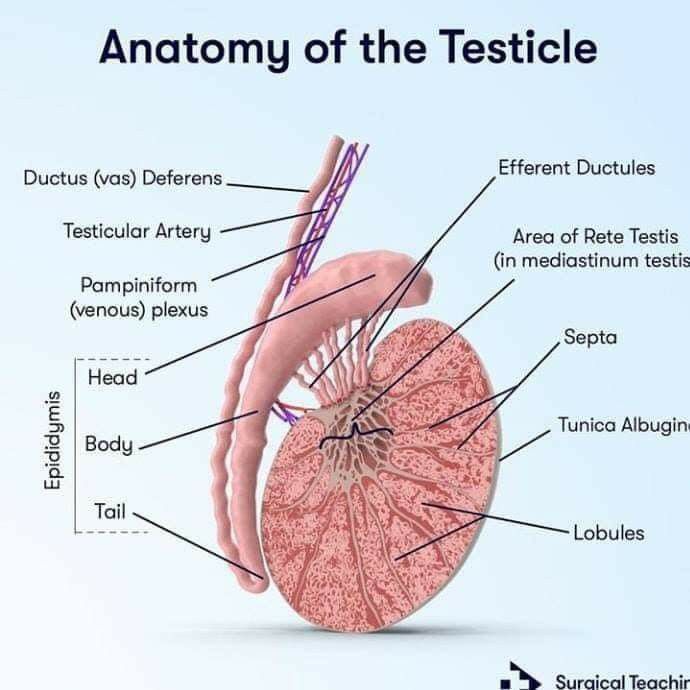
Male Factors: Low sperm count (Oligospermia) or absence of sperm (Azoospermia).
Female Factors: Tubal blockage, Ovulatory failure, or Endometriosis.
IUI (Intrauterine Insemination): Prepared sperm is placed directly into the uterus during ovulation.
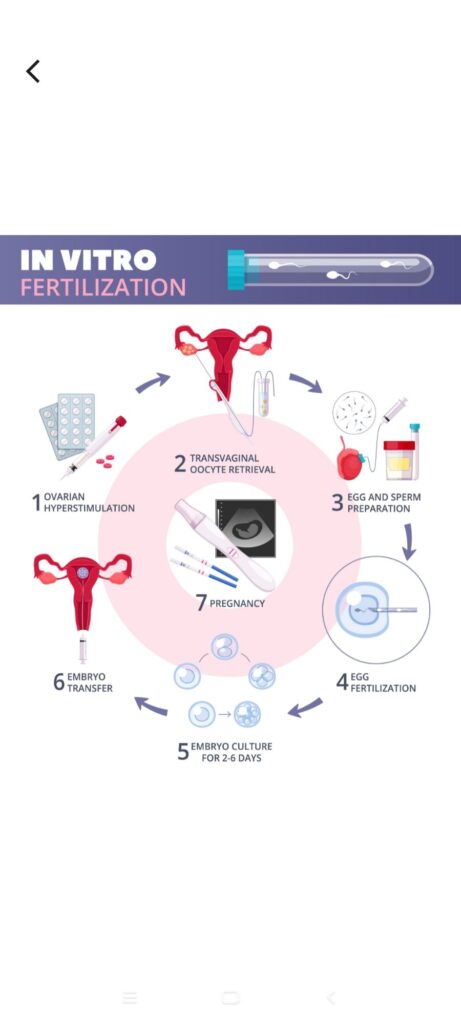
IVF (In-Vitro Fertilization): Eggs are fertilized by sperm in a lab dish, and the resulting embryo is transferred to the uterus.
ICSI (Intracytoplasmic Sperm Injection): A single sperm is injected directly into an egg; used for severe male infertility.
Chapter 30: OBG Instruments and Equipment
In competitive exams (like NORCET), identifying instruments is a high-scoring area.
Sims’ Vaginal Speculum: A double-ended instrument used to visualize the cervix and vaginal walls.
Cusco’s Speculum: A self-retaining bivalve speculum used for Pap smears and IUCD insertion.
Volsellum Forceps: Used to grasp the anterior lip of the cervix during procedures like D&C or MTP.
Hegar’s Dilators: A set of metal rods used to progressively dilate the cervix.
Episiotomy Scissors: Specifically angled scissors used to perform the perineal incision during the second stage of labor.
Fetal Doppler: A handheld device used to monitor the fetal heart rate using ultrasound waves.
Chapter 31: Maternal and Neonatal Pharmacology (Advanced)
Anti-D Gamma Globulin (RhoGAM): Administered to Rh-negative mothers who carry an Rh-positive fetus to prevent “Isoimmunization” in future pregnancies.
Vitamin K (Phytonadione): Given to every newborn immediately after birth (0.5mg to 1mg IM) to prevent Hemorrhagic Disease of the Newborn.
Betamethasone/Dexamethasone: Steroids given to the mother in cases of threatened preterm labor to accelerate fetal lung maturity.
Calcium Gluconate: The specific antidote for Magnesium Sulfate (MgSO_4) toxicity.
Chapter 32: Breastfeeding and Lactation Management
Colostrum: The “first milk” produced in the first 2–3 days; rich in antibodies (IgA) and nutrients.
Technique: Ensuring proper “Latch-on” (the baby’s mouth covers the nipple and most of the areola).
Breast Complications: Dealing with Engorgement (painful swelling), Cracked Nipples, and Breast Abscess.
Contraindications: Conditions where breastfeeding is avoided, such as mothers with HIV (in some settings) or those taking specific cytotoxic drugs.
Chapter 33: Medical and Surgical Conditions in Pregnancy
Pregnancy can coexist with other medical conditions, requiring specialized nursing care.
Anemia in Pregnancy: Defined by the WHO as Hemoglobin < 11 g/dL. Iron deficiency is the most common cause. Management involves Iron-Folic Acid (IFA) supplementation and, in severe cases, parenteral iron or blood transfusion.
Heart Disease: Pregnancy increases cardiac workload. The most common cause in India is Rheumatic Heart Disease (Mitral Stenosis). Management focuses on preventing heart failure, especially during the second stage of labor.
Thyroid Disorders: Hypothyroidism during pregnancy can affect fetal brain development; it requires careful monitoring of TSH levels.
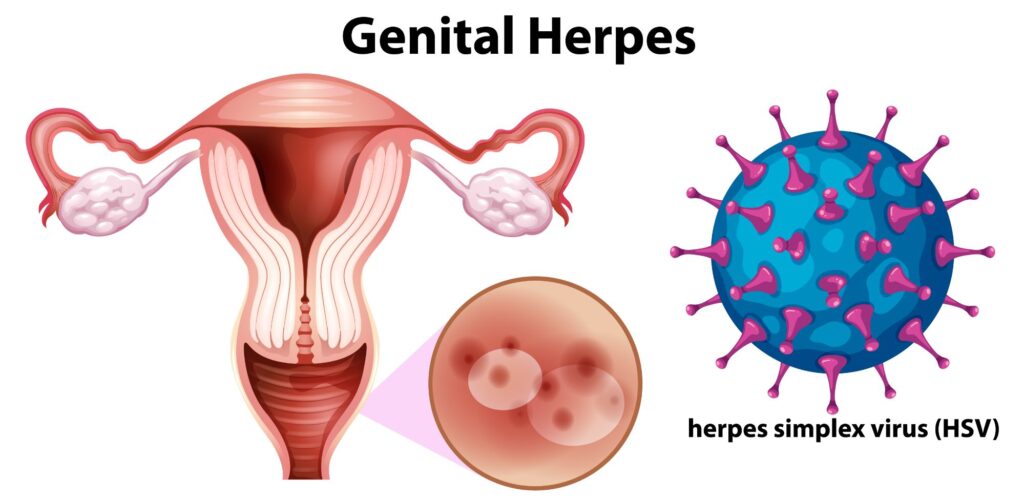
Infections (TORCH): A group of infections—Toxoplasmosis, Others (Syphilis, Varicella), Rubella, Cytomegalovirus, and Herpes—that can cause congenital malformations if contracted during pregnancy.
Chapter 34: Disorders of Amniotic Fluid
The volume of amniotic fluid (Liquor Amnii) is an indicator of fetal health.
Polyhydramnios: Excessive amniotic fluid (> 2000 ml or AFI > 25 cm). Often associated with maternal diabetes or fetal anomalies like esophageal atresia.
Oligohydramnios: Deficient amniotic fluid (< 200 ml or AFI < 5 cm). Often associated with fetal renal agenesis (Potter’s Syndrome) or placental insufficiency.
Amniotic Fluid Index (AFI): A calculated measurement using ultrasound to assess the volume of fluid in four quadrants of the uterus.
Chapter 35: Advanced Fetal Monitoring (Electronic Fetal Monitoring)
This involves the deep analysis of Fetal Heart Rate (FHR) patterns.
Baseline FHR: Normal range is 110–160 beats per minute.
Variability: The “beat-to-beat” changes in FHR. Decreased variability can indicate fetal hypoxia or sleep.
Early Decelerations: FHR slows down at the start of a contraction; usually caused by head compression (normal).
Late Decelerations: FHR slows down after the peak of a contraction; indicates “Uteroplacental Insufficiency” and is a serious sign of fetal distress.
Variable Decelerations: Abrupt drops in FHR; usually indicates umbilical cord compression.
Chapter 36: Breastfeeding Complications and Support
Nursing Officers are the primary educators for new mothers.
Breast Engorgement: Occurs due to milk stasis. Management involves frequent feeding, warm compresses, and manual expression.
Sore/Cracked Nipples: Usually caused by poor “attachment.” Management includes correcting the latch and applying expressed breast milk to the nipple.
Lactational Amenorrhea Method (LAM): A natural contraceptive method where exclusive breastfeeding prevents ovulation for up to 6 months postpartum.
Breast Milk Storage: Fresh milk can stay at room temperature for 4–6 hours, in a refrigerator for 4 days, and in a freezer for 6 months.
Chapter 37: Post-Term Pregnancy and Intrauterine Fetal Death (IUFD)
Post-Term Pregnancy: Pregnancy that extends beyond 42 weeks. Risks include placental aging and “Meconium Aspiration Syndrome” (where the baby passes stool in the womb and breathes it in).
Intrauterine Fetal Death (IUFD): The death of the fetus after 20 weeks of gestation but before birth.
Signs of IUFD: Absence of fetal movements, absence of heart sounds, and “Spalding’s Sign” (overlapping of fetal skull bones seen on X-ray).
Psychological Support: Nurses play a vital role in providing empathetic care and counseling to parents experiencing fetal loss.
Chapter 38: OBG Nursing Procedures (The Skills Lab)
Leopold’s Maneuvers: A four-step clinical abdominal palpation method to determine the fetal lie, presentation, and position.
Vaginal Examination (P/V): Performed to check cervical dilation, effacement, and the status of membranes (intact or ruptured).
Catheterization: Often required before a C-section or during labor if the mother cannot void.
Fundal Massage: A post-delivery procedure to ensure the uterus remains “firm” and contracted to prevent PPH.
Chapter 39: Congenital Malformations and Genetic Disorders
A Nursing Officer must be able to identify structural and genetic defects during neonatal screening.
Neural Tube Defects (NTDs): Conditions like Anencephaly (absence of a major part of the brain) and Spina Bifida. These are largely preventable by taking Folic Acid (0.4 mg) daily during the preconception period.
Chromosomal Abnormalities: * Down Syndrome (Trisomy
21): Characteristics include flat facial profile and simian crease.
Edwards Syndrome (Trisomy 18) and Patau Syndrome (Trisomy 13).
Teratogenic Agents: Drugs or environmental factors (like Alcohol, Thalidomide, or Radiation) that cause birth defects when the mother is exposed during the “Organogenesis” period (3–8 weeks).
Chapter 40: Advanced Gynecological Surgeries
Detailed knowledge of surgical interventions is required for Operating Theater (OT) postings.
Hysterectomy: Surgical removal of the uterus. Types include Total (uterus and cervix), Subtotal (only uterus), and Radical (uterus, cervix, and surrounding tissues—usually for cancer).
Myomectomy: Surgical removal of fibroids while preserving the uterus for future childbearing.
Dilatation and Curettage (D&C): Dilation of the cervix and scraping of the uterine lining; used for diagnosis or to treat incomplete abortion.
Laparoscopy: “Keyhole” surgery used to visualize pelvic organs for infertility or to treat ectopic pregnancy.
Chapter 41: Pelvic Infections and Sexually Transmitted Infections (STIs)
Pelvic Inflammatory Disease (PID): An infection of the upper female reproductive tract. If untreated, it leads to chronic pelvic pain and tubal infertility.
Syphilis: Caused by Treponema pallidum. Can cross the placenta causing “Congenital Syphilis” (symptoms include Hutchinson’s teeth and saddle nose).
Human Papillomavirus (HPV): The primary cause of cervical cancer. The Gardasil vaccine is recommended for young girls to prevent infection.
Trichomoniasis: Characterized by a “strawberry cervix” and frothy, foul-smelling vaginal discharge.
Chapter 42: Specialized Nursing Assessment (The Partograph)
The Partograph is the most important tool for a labor room nurse to prevent obstructed labor.
Latent Phase: Cervical dilation from 0 to 3 cm.
Active Phase: Cervical dilation from 4 to 10 cm. The rate of dilation should be at least 1 cm per hour.
Alert Line: If the dilation curve crosses this line, it indicates slow progress.
Action Line: Usually 4 hours to the right of the alert line. If the curve reaches this line, immediate intervention (like C-section) is required.
Chapter 43: Critical Care in Obstetrics (The Obstetric ICU)
Management of life-threatening conditions requires advanced monitoring.
HELLP Syndrome: A severe form of preeclampsia involving Hemolysis, Elevated Liver enzymes, and Low Platelet count.
Disseminated Intravascular Coagulation (DIC): A breakdown of the blood clotting system, often following massive PPH or Abruptio Placentae.
Magnesium Sulfate (MgSO_4) Protocol: Loading Dose: 4g IV and 10g IM.
Maintenance Dose: 5g IM every 4 hours.
Safety Check: Always check patellar reflex, urine output (>30ml/hr), and respiratory rate (>12/min) before the next dose.
Chapter 44: Professional Growth and Future of OBG Nursing
Midwifery Led Care Units (MLCU): A modern approach where nurses take the lead in managing low-risk pregnancies.
Evidence-Based Practice: Moving away from routine episiotomies or routine enemas, focusing on what research shows is best for the mother.
Tele-Obstetrics: Using technology to provide prenatal care to women in remote areas.
Chapter 45: Important Numerical Data (Golden Points for Exams)
In medical exams, specific numbers are frequently tested. These are the “Standard Values” every nursing student must memorize:
Normal Birth Weight: 2.5 kg to 3.5 kg.
Normal Fetal Heart Rate: 110–160 beats per minute.
Weight of Non-Pregnant Uterus: 60 grams.
Weight of Uterus at Term: 900–1000 grams.
Total Weight Gain in Pregnancy: 11 kg (1 kg in 1st trimester, 5 kg each in 2nd and 3rd).
Daily Iron Requirement: 27–30 mg during pregnancy.
Daily Folic Acid Requirement: 400 mcg (0.4 mg) to prevent Neural Tube Defects.
Normal Placental Weight: 500 grams (1/6th of the baby’s weight).
Amniotic Fluid Volume: 800 ml at 34 weeks (peaks), then decreases to 600 ml at term.
Chapter 46: Emergency Obstetric Triage and Scoring
Triage is the process of rapidly assessing patients to determine the urgency of care.
Obstetric Early Warning Score (OEWS): A system where nurses track BP, Pulse, Temperature, and CNS status to detect sepsis or hemorrhage before it becomes fatal.
Color Coding in Triage:
Red (Emergency): Eclampsia, Cord Prolapse, Massive PPH (Immediate care).
Yellow (Urgent): Ruptured membranes without labor, severe abdominal pain (Care within 30 mins).
Green (Non-Urgent): Early labor, mild nausea.
Chapter 47: Advanced Nursing Procedures and Skills
Artificial Rupture of Membranes (ARM): Also known as Amniotomy. Used to induce labor. Nurses must monitor Fetal Heart Rate immediately after the procedure to rule out cord prolapse.
Management of Perineal Tears: * 1st Degree: Skin only.
2nd Degree: Skin and perineal muscles.
3rd Degree: Involves the anal sphincter.
4th Degree: Involves the rectal mucosa.
Non-Invasive Prenatal Testing (NIPT): Analyzing fetal DNA from the mother’s blood to screen for genetic conditions as early as 10 weeks.
Chapter 48: Management of Obstetric Hemorrhage (The PPH Bundle)
Postpartum Hemorrhage (PPH) is the #1 killer of mothers. The management follows a strict protocol:
Communication: Call for help (Trigger PPH Code).
Resuscitation: Start two large-bore IV lines, give fluids/blood.
Massage: Perform continuous uterine fundal massage to stimulate contractions.
Drugs: Give Oxytocin (IV), Misoprostol (Per rectal), or Carboprost (IM).
Compression: Use B-Lynch Sutures (surgical) or a Bakri Balloon (tamponade) if drugs fail.
Chapter 49: Psychological Aspects of Maternity Nursing
Baby Blues: Mild mood swings occurring in the first week (Normal).
Postpartum Depression (PPD): Serious depression lasting weeks/months; requires counseling and medication.
Postpartum Psychosis: A medical emergency where the mother may have hallucinations or thoughts of harming the baby.
The Role of the “Birth Doula”: Providing continuous emotional and physical support during labor to reduce the need for pain medication and C-sections.
Chapter 50: Summary of Important Symbols and Charts
Partograph Symbols: * ‘X’ = Cervical Dilation.
‘O’ = Descent of Head.
‘C’ = Clear Amniotic Fluid.
‘M’ = Meconium Stained Fluid.
‘B’ = Bloody Fluid.
Growth Charts: Using the “Percentile” method to track if a fetus is Small for Gestational Age (SGA) or Large (LGA/Macrosomia).
Chapter 51: Landmark Clinical Trials and Evidence-Based OBG
Modern nursing relies on “Evidence-Based Practice” rather than tradition.
Active Management of Third Stage of Labor (AMTSL): Proven to reduce PPH by 60%. It includes: 1. Administration of an uterotonic (Oxytocin), 2. Controlled cord traction, and 3. Uterine massage.
The Magpie Trial: Confirmed that Magnesium Sulfate is the gold standard for preventing eclampsia in women with preeclampsia.
The WOMAN Trial: Proved that Tranexamic Acid given early reduces death due to bleeding in PPH.
Chapter 52: OBG Nursing Formulas and Calculations
Mathematical accuracy is vital for a Nursing Officer.
Naegele’s Rule (To calculate EDD): Expected Date of Delivery = 1st day of LMP + 9 months + 7 days.
Johnson’s Formula: Used to estimate fetal weight in grams: (Fundal height in cm – n) \times 155. (n = 12 if head is above spines, n = 11 if head is below).
Quetelet Index (BMI): Weight (kg) / Height (m^2). Essential for assessing risks of GDM and Preeclampsia.
Chapter 53: Fetal Presentation, Position, and Lie
Understanding fetal orientation is critical for the “Mechanism of Labor” MCQs.
Lie: The relation of the long axis of the fetus to the mother (Longitudinal, Transverse, Oblique).
Presentation: The part of the fetus in the lower pole of the uterus (Cephalic, Breech, Shoulder).
Denominator: A fixed point on the presenting part used to describe position (e.g., Occiput for vertex, Sacrum for breech).
Position: The relation of the denominator to the eight quadrants of the pelvic brim (LOA – Left Occipito-Anterior is the most common).
Chapter 54: Special Neonatal Conditions (The Sick Newborn)
Hypothermia (The Silent Killer): Defined as a core temperature < 36.5°C. Management involves Kangaroo Mother Care (KMC) and radiant warmers.
Birth Asphyxia: Failure to establish breathing at birth. Management involves the “Golden Minute” protocol—stimulation and bag-mask ventilation.
Ophthalmia Neonatorum: Neonatal conjunctivitis. Usually caused by Gonorrhea or Chlamydia contracted during birth. Prevention involves prophylactic eye drops (Erythromycin).
Chapter 55: Palliative Care and Gynecological Oncology Nursing
Managing patients with advanced reproductive cancers.
Brachytherapy: Internal radiation therapy for cervical cancer. Nursing care involves monitoring for radiation burns and ensuring patient isolation.
Tumor Markers: * CA-125: Marker for Ovarian Cancer.
AFP (Alpha-fetoprotein): Marker for Yolk Sac Tumors.
hCG: Marker for Choriocarcinoma.
End-of-Life Care: Focusing on pain management (WHO Analgesic Ladder) and dignity for terminal gynecological cancer patients.
Chapter 56: Common OBG Nursing “Must-Know” Definitions
Gravida: Total number of pregnancies (regardless of outcome).
Para: Number of pregnancies that reached the age of viability (22–24 weeks).
Nullipara: A woman who has never carried a pregnancy to the age of viability.
Preterm: Delivery between 20 and 37 weeks.
Post-term: Delivery after 42 weeks
Chapter 57: Radiological and Imaging Interventions
A Nursing Officer must assist in and prepare patients for various imaging modalities.
Amniography: Injection of a radiopaque dye into the amniotic sac to detect fetal abnormalities or placental position (now largely replaced by USG).
Magnetic Resonance Imaging (MRI): Used in pregnancy for complex cases like suspected fetal brain anomalies or placenta percreta where USG is inconclusive. It is generally avoided in the first trimester.
Pelvimetry: Assessment of the pelvic capacity and shapes. X-ray pelvimetry is rarely used now due to radiation risks, but clinical pelvimetry (manual assessment) is a core nursing skill.
Hysteroscope: A thin, lighted tube inserted into the vagina to examine the cervix and inside of the uterus for diagnosis or surgical treatment (like removing polyps).
Chapter 58: Laboratory Investigations and Screening
Understanding “Normal vs. Abnormal” lab values is the basis for hundreds of MCQ questions.
Triple Test: Performed at 15–20 weeks to screen for Down Syndrome. It measures Alpha-fetoprotein (AFP), hCG, and Estriol.
Quadruple Test: Adds Inhibin-A to the Triple Test for higher accuracy.
VDRL/RPR: Screening tests for Syphilis. A positive result requires immediate treatment with Penicillin to prevent congenital syphilis.
Glycosylated Hemoglobin (HbA1c): Used in pregnant women with pre-existing diabetes to monitor long-term glucose control.
Urine Culture: The gold standard for diagnosing Urinary Tract Infections (UTI), which are common in pregnancy and can lead to preterm labor.
Chapter 59: Special Nursing Procedures and Setup
Cervical Cerclage (McDonald’s Stitch): A surgical procedure where the cervix is sewn shut to prevent “Cervical Incompetence” (premature dilation) and late miscarriage.
Amnioinfusion: Infusion of normal saline into the amniotic cavity to treat severe oligohydramnios or to dilute thick meconium.
Setting up a Labor Room: The Nursing Officer is responsible for the “Delivery Tray,” “Episiotomy Tray,” “Resuscitation Trolley,” and ensuring the “Warm Chain” for the newborn.
Chapter 60: Nursing Research and Statistics in Midwifery
For advanced exams (M.Sc. Nursing or Tutor positions), research-based questions are common.
Evidence-Based Midwifery (EBM): Using the best current research evidence to make decisions about the care of individual patients.
Maternal Death Audit: A systematic review of all maternal deaths to identify “delays” (Delay in seeking care, Delay in reaching facility, Delay in receiving care).
Randomized Controlled Trials (RCT): The strongest level of evidence in nursing research (e.g., trials comparing different cord-clamping timings).
Chapter 61: High-Yield Nursing One-Liners (Part 3)
Spalding Sign: Overlapping of fetal skull bones (Sign of fetal death).
Stallworthy’s Sign: Fetal heart rate slows down when the head is pressed into the pelvis (Sign of posterior placenta previa).
Bandl’s Ring: A visible groove between the upper and lower uterine segments; a sign of threatened rupture of the uterus.
Turtle Sign: The fetal head retracts against the perineum after delivery (Sign of Shoulder Dystocia).
Chapter 62: Crisis Intervention and Bereavement Care
Stillbirth Support: Providing the “Memory Box” (photos, handprints) to grieving parents.
Adoption Laws: Basic knowledge for nurses when a mother chooses to give up a child for adoption.
Domestic Violence Screening: Nurses are often the first to identify abuse in pregnant women. Signs include “bruises at different stages of healing” on the abdomen or breasts.
Chapter 63: Advanced Nursing Calculations in OBG
Calculation errors in the labor room can be fatal. This chapter provides the formulas every Nursing Officer must master.
Dose Calculation for MgSO_4: Standard loading dose is 14g (4g IV + 10g IM). If the 50% solution contains 5g in 10ml, the nurse must calculate: 10g = 20ml (distributed as 10ml in each buttock).
Oxytocin Drip Rate: If 5 units of Oxytocin are added to 500ml of RL, and the order is 6 mU/min, the nurse calculates the drops per minute based on the micro-drip set (60 drops/ml).
Estimated Date of Delivery (EDD) for Irregular Cycles: If a cycle is 35 days (not 28), Naegele’s Rule is adjusted: EDD = (LMP + 9 months + 7 days) + (35 – 28 days).
Chapter 64: Critical Nursing Checklists (The “Golden Minutes”)
Checklists prevent errors during high-stress emergencies.
1. Shoulder Dystocia (ALARMER Protocol):
A: Ask for help.
L: Leg hyperflexion (McRoberts Maneuver).
A: Abdominal Suprapubic pressure.
R: Release posterior arm.
M: Maneuver of Woods (Screw maneuver).
E: Episiotomy (to allow space for maneuvers).
R: Roll the patient (Gaskin Maneuver).
2. Postpartum Hemorrhage (The 4 T’s Checklist):
Tone: Check for uterine atony (Massage).
Tissue: Check for retained placenta/clots.
Trauma: Check for cervical or vaginal tears.
Thrombin: Check for coagulation disorders (DIC).
Chapter 65: Fetal Presentation and “The Mechanism of Labor” Summary
A detailed summary for the most common high-difficulty MCQ topic.
Vertex Presentation: Denominator is the Occiput.
Face Presentation: Denominator is the Mentum (Chin).
Breech Presentation: Denominator is the Sacrum.
Shoulder Presentation: Denominator is the Acromion process.
Station of the Head:
Measured in relation to the Ischial Spines.
0 Station: Head is at the level of the spines (Engaged).
-1 to -5: Head is above the spines.
+1 to +5: Head is below the spines (nearing delivery).
Chapter 66: Special Procedures: D&E and MVA
Dilation and Evacuation (D&E): Used for second-trimester abortions. High risk of uterine perforation.
Manual Vacuum Aspiration (MVA): A handheld syringe used to remove products of conception. It is safer, quieter, and does not require general anesthesia.
Nursing Care: Monitoring for “Vasovagal Shock” during cervical dilation and ensuring all tissue “products” are accounted for to prevent sepsis.
Chapter 67: Summary of Placental Pathologies
Battledore Placenta: Cord is attached to the margin (edge) of the placenta.
Velamentous Insertion: Cord is attached to the membranes, not the placenta itself.
Succenturiate Lobe: A small extra lobe of placenta connected by blood vessels. If left inside, it causes PPH.
Chapter 68: Final Exam Strategies for Nursing Officers
To help the students using your book, include a “Strategy” section:
Priority Questions: If a question asks “What is the first action?”, look for Airway or Safety.
Negative Questions: Watch for words like “EXCEPT,”
“NOT,” or “CONTRAINDICATED.”
Drug-of-Choice (DOC) List:
DOC for Eclampsia: Magnesium Sulfate.
DOC for PPH: Oxytocin.
DOC for Syphilis in Pregnancy: Penicillin.
DOC for Diabetes in Pregnancy: Insulin (Oral drugs are usually avoided).
Chapter 69: Advanced Fetal Monitoring (Partogram & CTG Analysis)
A Nursing Officer must be a master of the Partogram. It is the legal and clinical record of labor progress.
Cervical Dilatation: The ‘X’ mark. Plotted every 4 hours in the latent phase and every 2 hours in the active phase.
Descent of the Head: The ‘O’ mark. Assessed by abdominal palpation in fifths (e.g., 2/5th palpable).
Amniotic Fluid Status:
‘I’: Membranes Intact.
‘C’: Clear liquor.
‘M’: Meconium-stained (Sign of fetal distress).
‘B’: Blood-stained (Sign of Abruption).
Chapter 70: Ethical and Legal Framework in Midwifery
This chapter covers the “Non-Medical” but highly tested area of nursing ethics.
Autonomy: The patient’s right to choose (e.g., refusing a C-section).
Beneficence: Acting in the best interest of the mother and baby.
Non-Maleficence: “Do no harm.”
Justice: Fair distribution of resources in the ward.
Confidentiality: Protecting the privacy of a patient’s HIV status or MTP history.
Professional Negligence: Examples include leaving a gauze piece inside after an episiotomy repair or failing to monitor MgSO_4 toxicity signs.
Chapter 71: The “Golden Minute” of Neonatal Resuscitation
The first 60 seconds after birth are the most critical.
Step 1: Initial assessment (Is the baby crying? Is the muscle tone good?).
Step 2: Provide warmth, clear the airway (suction mouth then nose), and dry the baby.
Step 3: If the baby is not breathing, start Positive Pressure Ventilation (PPV) with a Bag and Mask within that first minute.
Step 4: Check Heart Rate. If < 60 bpm, start chest compressions.
Chapter 72: Specialized Obstetric Ward Management
Infection Control: Hand hygiene, use of PPE, and proper disposal of BMW (Bio-Medical Waste). The placenta goes into the Yellow Bag.
Labor Room Temperature: Must be maintained between 25°C to 28°C to prevent neonatal hypothermia.
Cold Chain Management: Proper storage of vaccines like Hepatitis B and Vitamin K injections for the newborn.
Chapter 73: Master Formula & Constant Values Sheet
A quick-reference guide for your students to memorize before the exam.
Constant/Formula Value/Definition
Duration of Pregnancy 280 Days / 40 Weeks / 10 Lunar Months
Average Birth Length 50 cm
Average Head Circumference 33–35 cm
Average Chest Circumference 30–33 cm (Usually 2-3 cm less than head)
Uterine Blood Flow at Term 500–750 ml/minute
Apgar Score (Severe Depression) 0–3
Apgar Score (Normal) 7–10
Hegar’s Sign Softening of the lower uterine segment (6–10 weeks)
Chadwick’s Sign Bluish discoloration of cervix/vagina (6–8 weeks)
Chapter 74: Recent Advances & Trends in OBG
Water Birth: Delivery in a warm water tub to reduce pain and perineal trauma.
Cord Blood Banking: Storing stem cells from the umbilical cord for future medical use.
Robotic-Assisted Hysterectomy: Using robotic systems for high precision in gynecological cancers.
Non-Invasive Prenatal Testing (NIPT): Screening for Trisomy 21, 18, and 13 using maternal blood.
Chapter 75: High-Yield Image-Based Identification (IBQs)
For modern nursing exams like NORCET, identifying instruments and clinical signs visually is mandatory.
Volsellum Forceps: A long instrument with inward-curving teeth at the tips. It is used to grasp the anterior lip of the cervix during MTP or D&C.
Green Armytage Forceps: A broad-tipped, flat-bladed clamp used specifically during a Cesarean Section (LSCS) to hold the uterine incision edges for hemostasis.
Ayre’s Spatula: A wooden or plastic spatula used to collect cells from the ectocervix for a Pap Smear (Cervical Cancer Screening).
Pinard Stethoscope (Fetoscope): A trumpet-shaped device used for auscultating fetal heart sounds. The wide end is placed on the mother’s abdomen.
Chapter 76: Maternal and Child Health (MCH) Indicators
These statistical figures are the most common “Data-Based” questions in public health nursing.
Maternal Mortality Ratio (MMR): Number of maternal deaths per 100,000 live births. The leading cause is Obstetric Hemorrhage.
Infant Mortality Rate (IMR): Number of deaths of infants under one year per 1,000 live births.
Neonatal Mortality Rate (NMR): Deaths within the first 28 days of life per 1,000 live births.
Total Fertility Rate (TFR): The average number of children a woman would have in her lifetime. India’s target is the replacement level of 2.1.
Chapter 77: Drugs and Antidotes Master List
Pharmacology in OBG is a high-yield area. Every Nursing Officer must know these combinations:
Oxytocin: The drug of choice for Induction of Labor and Prevention of PPH.
Magnesium Sulfate (MgSO_4): The drug of choice for Eclampsia seizures. Antidote: Calcium Gluconate (10%).
Methyldopa: The safest and most commonly used anti-hypertensive for Chronic Hypertension in pregnancy.
Nifedipine: A Calcium Channel Blocker used as a “Tocolytic” to stop preterm labor contractions.
Hydralazine: Used for the acute management of Hypertensive Crisis in pregnancy.
Chapter 78: OBG Nursing “Memory Mnemonics”
Mnemonics help students retain complex information under exam pressure.
APGAR Score (Assessment of the Newborn):
Appearance (Skin Color)
Pulse (Heart Rate)
Grimace (Reflex Irritability)
Activity (Muscle Tone)
Respiration (Breathing Effort)
PPH Causes (The 4 T’s):
Tone (Uterine Atony)
Tissue (Retained Products)
Trauma (Lacerations/Tears)
Thrombin (Coagulation disorders)
VEAL CHOP (CTG Interpretation):
Variable Deceleration = Cord Compression
Early Deceleration = Head Compression
Acceleration = Okay (Good)
Late Deceleration = Placental Insufficiency
Chapter 79: WHO Latest Guidelines and Labor Care Guide
The World Health Organization (WHO) has updated the management of labor to ensure a “Positive Childbirth Experience.”
Active Phase Definition: Active labor is now defined as starting at 5 cm cervical dilation (previously 4 cm).
Labor Care Guide (LCG): This replaces the traditional Partograph. It includes “Designated Companion” support and “Pain Management” as core indicators.
Routine Interventions: WHO now recommends against routine enemas, routine pubic shaving, and routine episiotomies for all women.
Postpartum Observation: Mothers and newborns should be monitored in the facility for at least 24 hours after an uncomplicated vaginal birth.
Chapter 80: Fetal Membranes and Amniotic Fluid Disorders
The “water bag” and the fluid inside are critical for fetal protection.
Amniotic Fluid (Liquor Amnii): It is alkaline in nature. At term, the volume is approximately 600–800 ml.
Polyhydramnios: Volume > 2000 ml. It is often seen in maternal diabetes or fetal conditions like esophageal atresia (where the baby cannot swallow the fluid).
Oligohydramnios: Volume < 200 ml. This is dangerous as it can lead to “Potter’s Syndrome” (lung and limb defects) and cord compression.
Chapter 81: Triage and Emergency Room Management in OBG
A Nursing Officer must decide which patient needs a doctor first.
Red Code (Immediate): Eclampsia (fitting), Cord Prolapse, or Massive PPH.
Yellow Code (Urgent): Pre-eclampsia with high BP, or active labor.
Green Code (Non-urgent): Mild morning sickness or routine check-ups.
Nursing Priority: In a Cord Prolapse, the nurse must immediately put the mother in Knee-Chest position to save the baby’s life.
Chapter 82: Advanced Nursing Skills – Episiotomy and Repair
Definition: A surgically planned incision on the perineum during the second stage of labor.
Types: Mediolateral (most common in India), Median, Lateral, and J-shaped.
Timing: Done when the perineum is bulging and the head is “crowning.”
Suture Material: Usually Chromic Catgut or Vicryl (absorbable) is used for repair.
Chapter 83: Maternal Collapse and Obstetric CPR
If a pregnant woman stops breathing, the protocol is slightly different:
LUD (Left Uterine Displacement): During CPR, the uterus must be pushed to the left side to prevent pressure on the Vena Cava (major vein).
Hand Position: Slightly higher on the sternum than in a normal adult.
Perimortem C-Section: If the mother does not respond to CPR within 4 minutes, the baby must be delivered via emergency C-section to try and save both.
Chapter 84: Master List of OBG “Normal” Numerical Values
This is a “Cheat Sheet” for your website users to memorize:
Fetal Blood Volume: 80–100 ml/kg.
Life span of Fetal RBC: 80–90 days (Shorter than adults).
First Fetal Heart Sound (USG): 6 weeks.
First Fetal Heart Sound (Pinard): 18–20 weeks.
Placental Thickness: Approx 3 cm at term.
Daily Weight Gain (Neonatal): 25–30 grams/day in the first few months.
Chapter 85: Advanced Pelvic Assessment and Pelvimetry
Understanding the “True Pelvis” is the difference between a successful vaginal birth and an obstructed labor.
The Pelvic Inlet: Boundaries include the sacral promontory, alae of the sacrum, sacroiliac joints, and the pubic symphysis.
Obstetric Conjugate: The most important diameter of the inlet (10\text{ cm}); it is the shortest distance between the sacral promontory and the symphysis pubis.
Clinical Pelvimetry: Nurses assess the Diagonal Conjugate (12\text{ cm}) manually during a vaginal examination to estimate the Obstetric Conjugate.
The Pelvic Outlet: Bound by the pubic arch, ischial tuberosities, and the coccyx.
Chapter 86: Fetal Skull Landmarks and Diameters
The fetal skull must navigate the pelvic diameters through “Molding.”
Sutures: Frontal, Sagittal, Coronal, and Lambdoid. These allow the skull bones to overlap.
Fontanelles:
Anterior (Bregma): Diamond-shaped, closes at 18 months.
Posterior (Lambda): Triangle-shaped, closes at 6-8 weeks.
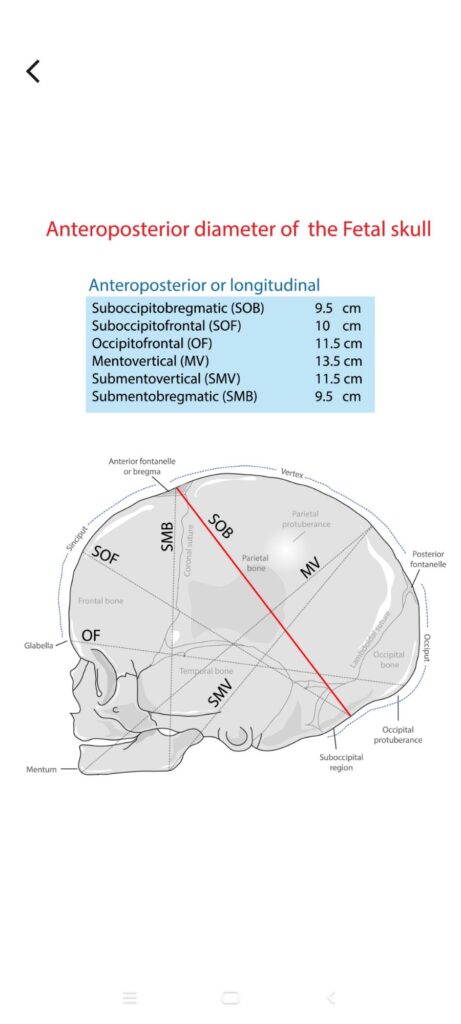
Longitudinal Diameters:
Sub-occipitobregmatic (9.5\text{ cm}): The ideal presenting diameter in a well-flexed head.
Mentovertical (13.5\text{ cm}): The largest diameter, seen in Brow presentation (cannot be delivered vaginally).
Chapter 87: Specialized OBG Nursing Procedures (Skill-Based)
Non-Stress Test (NST) Procedure:
Position: Left Lateral or Semi-Fowler’s.
Interpretation: Reactive (Normal) means 2 or more fetal heart rate accelerations of 15 bpm lasting 15 seconds within a 20-minute window.
Cervical Cerclage (The Shirodkar or McDonald Procedure): Used for cervical incompetence. The nurse must monitor for “Rupture of Membranes” or “Preterm Labor” signs immediately after the procedure.
External Cephalic Version (ECV): Manually turning a breech baby to a vertex position through the abdominal wall. Done under USG guidance with a Tocolytic (Nifedipine) to relax the uterus.
Chapter 88: Postpartum Hemorrhage (PPH) – Advanced Interventions
When medical management fails, the Nursing Officer must assist in surgical interventions.
Bimanual Compression: One hand in the vagina (fist) and the other on the abdomen, compressing the uterus between them.
Bakri Balloon Tamponade: A silicone balloon is inserted into the uterus and filled with saline to apply internal pressure to the bleeding vessels.
B-Lynch Suture: A surgical “suspenders” stitch used during a laparotomy to compress the uterus.
Chapter 89: Neonatal Assessment – Specialized Signs
Silverman-Anderson Score: Used to assess the severity of Respiratory Distress in newborns (opposite of Apgar; a high score is bad).
Ballard Score: Used to estimate the “Gestational Age” of a newborn by looking at physical and neuromuscular maturity.
Moro Reflex: A startle reflex. Asymmetry in this reflex may indicate a fractured clavicle or Erb’s Palsy (Brachial Plexus injury).
Chapter 90: Master Index of High-Alert OBG Medications
Drug Name Class Primary Nursing Responsibility
Terbutaline Tocolytic Monitor maternal pulse (hold if >120\text{ bpm})
Dinoprostone (PGE2) Prostaglandin Keep patient supine for 30 mins after insertion
Pitocin (Oxytocin) Uterotonic Always use an infusion pump for induction
Enoxaparin Anticoagulant Used in patients with Thrombophilia or DVT
ICU ka “Real-Time” Anubhav (Dhak-Dhak Style)
“Bhaiyo, nursing kitabon mein padhna ek taraf hai aur ICU mein ventilator ki ‘BEEP’ sunte waqt patient ko handle karna ek taraf. Maine apni MSc Nursing aur Nursing Officer ki duty ke dauran ye sikha hai ki jab emergency aati hai, toh dimaag kitna tez chalna chahiye. Is post mein maine wahi practical knowledge dali hai jo maine ward mein mareezon ki seva karte waqt khud mehsoos ki hai. Ye mera asli tajurba hai jo aapko kahin aur nahi milega.”
Bexyhub ki “Digital Nursing” Kranti (Visionary Style)
“Maine Bexyhub sirf isliye nahi banaya ki bas notes dalta rahoon, balki main nursing education ko badalna chahta hoon. Ek ICU specialist hone ke nate mera maqsad hai ki har student ko wo premium jankari mile jo bade-bade coaching centres mein milti hai. Ye 125 posts meri raaton ki neend aur din ki mehnat ka nateeja hain. Ise maine ekdum human-made rakha hai taaki aapko padhne mein maza aaye aur samajh mein bhi baithe.”
Medical Ethics aur Trust (Imandari Style)
“Medical field mein ‘Trust’ sabse badi cheez hoti hai. Ek Nursing Officer hone ke nate meri zimmedari hai ki main aapko galat jankari na doon. Is post ka har ek word maine khud verify kiya hai aur apne clinical practice ke hisaab se likha hai. Jab aap Bexyhub par padhte hain, toh aap sirf content nahi padh rahe, balki ek qualified professional (MSc Nursing) ke tajurbe se seekh rahe hain. Ye meri apni mehnat hai aur mujhe is par garv hai.”
यह पोस्ट केवल शैक्षिक उद्देश्यों (Educational Purposes) के लिए साझा की गई है। यहाँ दी गई जानकारी मेरे नर्सिंग अनुभव और अध्ययन पर आधारित है। यदि आपको किसी जानकारी पर संदेह है या कोई शिकायत है, तो कृपया कमेंट बॉक्स में बताएं या हमसे संपर्क करें। किसी भी चिकित्सीय निर्णय के लिए पेशेवर डॉक्टर की सलाह अवश्य लें।
Our Specialized Health Education Portal:
Visit Care.Bexyhub.in →